News & Announcements
Two Decades of Innovation
Oct. 6, 2020
Twenty years ago, the School of Health Related Professions was a unit within the School of Medicine. Many of its programs, which enrolled just over 500 students a year, were hospital-based. The school had limited resources and lacked the capacity to expand. And the term “related” left a bad taste in the mouth of many faculty members. The time was right for a new identity.
The faculty, spearheaded by Director Richard Oliver, BS MT ’71, M Ed ’73, PhD ’77, petitioned the board of curators to become a freestanding school, and in 2001, the School of Health Professions was born.
“When a university has the ability to respond to societal needs, we have an obligation to explore how we do that,” Oliver says. “We wanted to help solve widespread dilemmas that families face — whether you’re a child with speech difficulties or a senior who isn’t getting adequate services.”
Today, the school’s faculty are leaders in cutting-edge research in health disparities, language development, autism interventions and stroke rehabilitation. Working alongside faculty in multiple outpatient clinics, students get hands-on experience and conduct their own research while providing much-needed services to the community. Following graduation, alumni become leaders in their fields and help shape the future of health care delivery in Missouri and beyond.
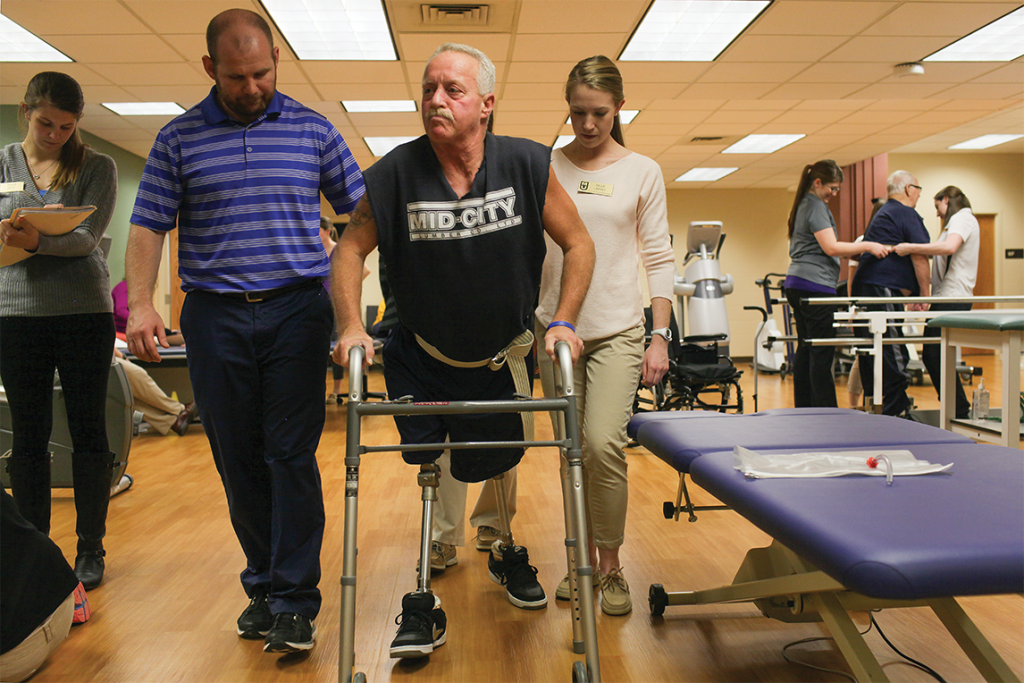
Bringing Discovery to the Community
In the early 2000s, Laura Schopp, MA ’91, PhD ’95, was training rural psychologists to provide brain injury services using telehealth video conferencing when her postdoctoral fellow pointed out that audio and video were not synchronized. For those who are hard of hearing, it would have been impossible to lip-read.
“We thought, oh, boy, that’s a problem,” recalls Schopp, a health psychologist and founding faculty member, now chair, of the school’s Department of Health Psychology. So, she recruited a team of engineers, and together, they won a National Institutes of Health grant to fix the problem. Researchers not only achieved synchronicity but also changed video compression so people could use sign language without the screen growing blurry. The improved technology also provided real-time captioning.
“It was a great opportunity to have a group of neuropsychologists and rehabilitation psychologists who were providing independent practice, doing research, and training interns and postdoctoral fellows become part of this new initiative,” says Kristofer Hagglund, who became dean in 2013. “They helped set the tone for the future in terms of research for the School of Health Professions.”
Research faculty from across seven departments and 13 disciplines tackle critical issues facing the health and well-being of children and adults in diverse populations. The agenda focuses on translational and entrepreneurial research in health restoration and rehabilitation as well as issues that pinpoint health disparities and health care delivery to vulnerable populations and people with chronic diseases.
In recent years, research productivity has surged. The National Institutes of Health has awarded health professions researchers $3.8 million to develop an autism measurement tool and more than $2.7 million to evaluate a new intervention to help stroke patients improve performance of everyday activities. Researchers have also received $2.8 million from the National Institute on Deafness and Other Communication Disorders to expand voice disorder research and $1.2 million from the Health Resources and Services Administration for clinical training of doctoral students in underserved Missouri communities affected by the opioid epidemic.
The common threads? The work is highly interdisciplinary, and the goal is to optimize individual and community health. Faculty not only collaborate within the School of Health Professions — “I have learned much more about nuclear medicine than most respiratory therapists,” says Kathy Moss, M Ed ’93, PhD ’15, chair of the clinical and diagnostic sciences department. They also team up with colleagues in nearly every school and college at MU. Speech pathologists work with computer scientists. Occupational therapists collaborate with electrical engineers. Health psychologists conduct research with neurologists.
“The opportunity to become a freestanding school allowed us to consolidate all of our strengths in the health professions so that cross-fertilization and collaboration could happen,” Schopp says.
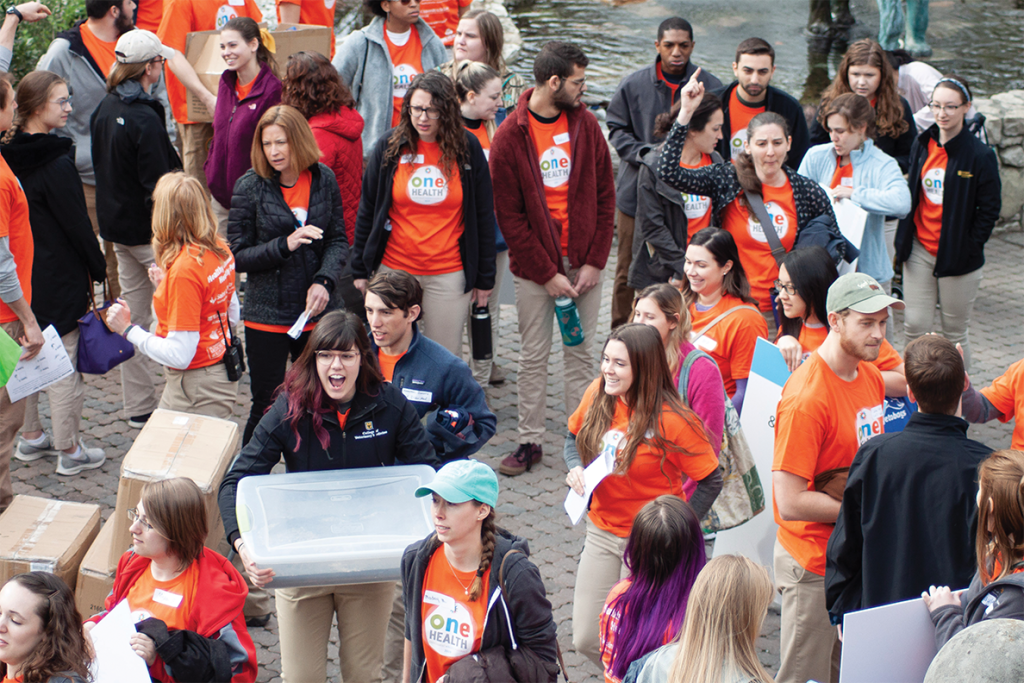
Educating the Backbone of the Health Care Workforce
To continue strengthening the school’s interdisciplinary research-focused graduate education, it introduced in 2019 Missouri’s only doctoral program in health and rehabilitation science at a public institution. That was just one of many new programs to come out of the School of Health Professions during the past two decades.
In 2007, the school joined forces with the College of Veterinary Medicine and School of Public Affairs to ask important questions, train the next generation of public health leaders and address the needs of underserved populations. Since its inception, the Master of Public Health program has graduated nearly 600 students. Many stay and work in the county and local agencies where they had their internships. Others head to the Centers for Disease Control and Prevention and the United States Department of Agriculture.
The school’s watershed event occurred, however, in 2009. In response to student demand and the growing shortage of health care professionals in Missouri, a team of faculty and student service members built a new major: health science. It provides students with a solid health care background, preparing them to pursue not only graduate or professional health science programs but also nonclinical careers. Students find jobs in everything from medical case management and human services to corporate wellness and pharmaceutical manufacturing.
“We’re not a technical training school,” Hagglund says. “We provide a strong liberal arts education that emphasizes health and health care.”
When the new degree launched, it was one of only a handful of programs of its kind nationwide, Hagglund says. Leaders anticipated that, within five years, they’d have 275 students. By 2013, more than 1,200 students had enrolled in the program. In 2017, it became the No. 1 major on campus, graduating 578 students in 2019, a majority of whom (69 percent) stay in Missouri.
“We’re training the next generation of health care professionals,” says Program Director Botswana Blackburn, BJ ’95, M Ed ’97, who received a Kemper Fellowship for Teaching Excellence in 2019. “Being a land-grant institution, we’re focused on making sure our students are culturally competent and can work in diverse populations so we’re meeting the needs of Missourians.”
Since 2001, the school has also created dozens of online programs and certificates and elevated the entry-level degree to doctorate for both the physical therapy and occupational therapy programs.
Now the fourth-largest school for enrollment at MU, the School of Health Professions has indeed forged its own identity. The school quickly became known for investing in clinical operations that provide the community with services and students with training and research opportunities.

Serving Today’s Families, Teaching Tomorrow’s Practitioners
For the School of Health Professions, improving the health of Missouri’s citizens has always been a central mission. For instance, MU Speech and Hearing Clinics started traveling across Missouri in the 1950s. In response to community demand for adult services, the school opened Eldercare in 1989, becoming the only state-licensed adult day health care program serving families in Columbia. (The program, later known as Adult Day Connection, recently closed due to COVID-19 concerns.)
The school’s shift to becoming a freestanding unit gave it the opportunity and resources to expand its clinical programs. In 2005, Lea Ann Lowery, BHS ’88, M Ed ’03, created a pediatric occupational therapy clinic that not only serves children but also provides students with hands-on experience. Working in teams, students learn to see patients and their health in context while developing interventions that support the person as a whole, not just the illness. “In clinic, I immediately saw that the students were beginning to learn and understand the things that I had been trying to teach them through paper cases but couldn’t,” Lowery says.
Now known as TigerOT, the program has expanded to include occupational therapy and life skills training for adults, adaptive swimming for children with autism spectrum disorders, and low-vision services for adults and children.
Following suit, in 2011, a group of doctoral physical therapy students established PhysZOU, a volunteer-based, student-run, faculty-supervised pro bono physical therapy clinic. In 2013, the clinic was added to the physical therapy curriculum, and student participation became mandatory.
“Such experiences give students an incredible confidence boost,” says Teresa Briedwell, BHS ’81, associate department chair of physical therapy. “By the time they get to their first full-time clinical, they’re already a step ahead.”
The school’s nationally recognized service centers also include a preschool that serves children ages 2 to 5 with speech and language difficulties.
Hagglund sees the school’s growth and success continuing to accelerate over the next 20 years. “We will play a critical role in community health and sophisticated team-based health care. That includes advancing workforce diversity and reducing health disparities,” he says. “When it comes to research, I predict that our school will more than double its productivity. And, who knows, maybe we will also obtain a new state-of-the-art facility.”
This story by Kelsey Allen, BA, BJ ’10, was originally published in the Fall 2020 issue of MIZZOU alumni magazine.
Featured in this post

Kristofer Hagglund
Dean

Botswana Blackburn
Health Sciences Department Chair and Teaching Professor

Teresa Briedwell
Associate Department Chair and Teaching Professor

Lea Ann Lowery
Clinical Professor
